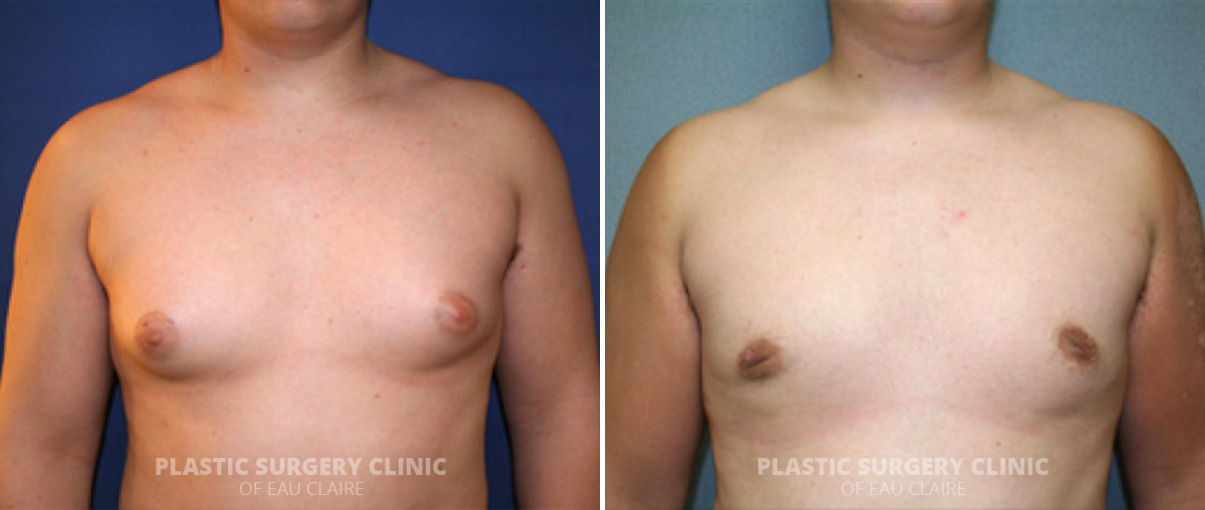
Are you a man living in Eau Claire, Wisconsin, who is struggling with the embarrassment of having enlarged breasts? If so, you are not alone. Gynecomastia, or male breast enlargement, is a common condition that affects many men. Fortunately, there is a solution: male breast reduction surgery. This article will explain gynecomastia and how it can be treated with male breast reduction surgery in Eau Claire, Wisconsin.

- What is Gynecomastia?
- What Causes Gynecomastia?
- How Common is Gynecomastia?
- Best Candidates for Gynecomastia
- The Male Breast Reduction Consultation
- Benefits of Male Breast Reduction Surgery
- Cost of Gynecomastia Surgery
- Performing Male Breast Reduction Surgery
- Risks of Gynecomastia Surgery
- The Expectations of Male Breast Reduction
- Recovery and Aftercare of Gynecomastia Surgery
- Frequently Asked Questions About Gynecomastia Surgery
What is Gynecomastia?
Gynecomastia is a condition that affects many men, causing enlarged breasts due to the presence of excess glandular breast tissue, fat deposits, and/or loose skin. In order to reduce the size of the breasts and create a more masculine chest appearance, male breast reduction surgery may be necessary. This surgical procedure removes excess glandular breast tissue, fat deposits, and/or loose skin from the chest area. This procedure aims to create a more contoured and aesthetically pleasing chest shape.
In some cases, Gynecomastia can be embarrassing due to its appearance. Many people want to reduce the size of their breasts for cosmetic purposes. That’s where Male Breast Reduction comes in! Male Breast Reduction effectively reduces the size of enlarged male breasts and makes them look more proportional.
We offer the latest techniques in Male Breast Reduction; our team is here to help you achieve your goals when it comes to reducing unwanted male breast tissue. We understand this can be a sensitive subject and will ensure your privacy and comfort throughout the process!
What Causes Gynecomastia?
Gynecomastia is caused by an imbalance of hormones, which can lead to glandular tissue growth in the chest area. This excess glandular tissue can cause the skin to stretch and enlarge, resulting in Gynecomastia. In some cases, Gynecomastia can be treated with lifestyle changes such as diet and exercise; however, in more severe cases, surgery may be necessary. Male Breast Reduction Surgery is a procedure that removes excess skin and glandular tissue from the chest area to reduce the size of enlarged male breasts.
In addition to Male Breast Reduction Surgery, there are other ways to reduce the size of enlarged male breasts. For example, weight loss can help reduce the amount of glandular tissue in the chest area and lead to a reduction in breast size. Additionally, certain medications can be used to inhibit breast development and help reduce the size of enlarged male breasts. It is important to talk with your doctor about any lifestyle changes or medications you may be considering before beginning any treatment plan.
Hormonal Imbalance
Hormonal imbalance is one of the most common causes of gynecomastia. When there is an imbalance between the hormones testosterone and estrogen, it can lead to an increase in breast tissue growth. This excess breast tissue can cause the chest area to become enlarged, resulting in gynecomastia. Male Breast Reduction Surgery is a procedure that removes excess skin and glandular tissue from the chest area to reduce the size of enlarged male breasts.
When considering Male Breast Reduction Surgery, it’s important to find a qualified plastic surgeon who has experience performing this type of procedure. A plastic surgeon will be able to assess your individual case and determine if surgery is right for you. During your consultation, they will discuss all aspects of the surgery, including possible risks and complications, as well as expected results. It’s also important to ask questions about any potential side effects or long-term effects that may occur after surgery.
Medications and Drugs
Certain medications and drugs can also cause Gynecomastia. These include certain antibiotics, anti-anxiety medications, steroids, and even some over-the-counter pain medications. If you are taking any of these medications and have noticed an increase in breast tissue growth, it’s important to talk to your doctor about the possibility of Gynecomastia. In some cases, switching to a different medication or reducing the dosage may be enough to reduce the size of enlarged male breasts. However, if this is not an option, Male Breast Reduction Surgery may be necessary.
Other Causes
Other causes of Gynecomastia include obesity, aging, and certain medical conditions such as kidney failure or liver disease. In some cases, these conditions can lead to an imbalance in hormones which can cause the growth of excess breast tissue. If you are suffering from any of these conditions and have noticed an increase in breast tissue growth, it’s important to talk to your doctor about the possibility of Gynecomastia. Male Breast Reduction Surgery may be necessary to reduce the size of enlarged male breasts.
How Common is Gynecomastia?
Gynecomastia is a fairly common condition, affecting up to 40% of men. It is caused by an imbalance in hormones, which can lead to fatty tissue growth in the chest area. Male Breast Reduction Surgery is a procedure that removes excess skin and fatty tissue from the chest area to reduce the size of enlarged male breasts. The procedure is relatively safe and effective, with most patients seeing results within a few weeks after surgery.
Best Candidates for Gynecomastia
When it comes to the best candidates for gynecomastia treatment, most men are ideal candidates. However, some factors can increase the likelihood of success with this procedure. For example, males who have been experiencing gynecomastia for over a year are usually good candidates for male breast reduction. This is because their breast tissue is sufficiently mature and has lessened in size and firmness as time passes.
It’s also important to note that individuals who suffer from extreme physical or psychological discomfort related to their gynecomastia are also good candidates for surgery. Candidates should be in general good health and meet the body fat requirements of trusted physician specialists. Lastly, those who want to reduce the amount of breast tissue they have while creating a more masculine appearance through their chest muscle definition may be better suited for this procedure than others.
Factors such as age, body fat percentage, and the amount of time you have been experiencing gynecomastia will all be taken into consideration when determining if you are a good candidate for gynecomastia surgery.
The Male Breast Reduction Consultation
If you’re considering getting a gynecomastia procedure in Eau Claire, Wisconsin, the first step is to have a consultation with your doctor. This will help you get an understanding of the procedures available and whether or not it’s the right choice for you. During this consultation, your doctor will also assess your physical health and identify any medical conditions that could complicate the surgery.
Your doctor may also ask to review some photographs of your chest area in order to get an idea of what results may be achievable from the male breast reduction surgery. Additionally, they’ll explain all potential risks associated with this operation so that you can make an informed decision about whether or not it’s right for you.
At the end of your gynecomastia consultation in Eau Claire, Wisconsin, your doctor should provide you with all the necessary information on how to prepare for your surgery as well as instructions on post-surgical care. This is important in helping ensure a smooth recovery process with minimal scarring and optimal results.
Benefits of Male Breast Reduction Surgery
- Gynecomastia surgery in Eau Claire, Wisconsin, can help reduce the size of enlarged male breasts and create a more masculine chest appearance.
- It can also help alleviate physical and psychological discomfort associated with gynecomastia.
- Male bret reduction surgery is relatively safe and effective, with most patients seeing results within a few weeks after surgery.
- The procedure can be tailored to each individual patient’s needs and goals, allowing for optimal results.
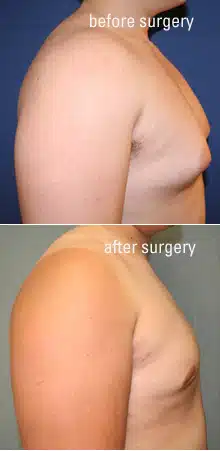
Procedure Before and After Photos
* Each patient is unique and individual results may vary.
Cost of Gynecomastia Surgery
The cost of male breast reduction surgery in Eau Claire, Wisconsin, can vary depending on the extent of the procedure and the patient’s individual needs. Generally speaking, the average cost for this type of surgery is between $3,000 and $5,000. However, some patients may qualify for financing options to help cover the costs. Additionally, insurance may cover some or all of the costs associated with surgical treatment for gynecomastia if it is deemed medically necessary.
For those looking to reduce their out-of-pocket expenses, a few options are available to breast reduction patients in Eau Claire. These include payment plans offered by some surgeons and discounts for cash payments or multiple procedures. It’s important to discuss these options with your doctor prior to scheduling your surgery so that you can make an informed decision about which option is best for you.
Performing Male Breast Reduction Surgery
When it comes to performing male breast reduction surgery in Eau Claire, Wisconsin, it is important to seek out a board-certified plastic surgeon who specializes in gynecomastia. This will ensure that the procedure is performed safely and effectively. During the breast reduction procedure, excess tissue and fat are removed from the chest area to create a more masculine appearance. The surgeon may also use liposuction techniques to further contour the chest area.
The board-certified plastic surgeon will discuss all aspects of the procedure with you beforehand, including potential risks and complications. They will also explain what you can expect during recovery and how long it may take for you to see results. It is important to follow all pre-operative instructions provided by your doctor in order to ensure a safe and successful outcome.
After the gynecomastia surgery is complete, patients typically experience some swelling and bruising around the chest area, which should subside within a few weeks after surgery. Patients should also wear compression garments for several weeks following their procedure in order to reduce swelling and help support their new chest shape as they heal. With proper care and attention, most patients can expect excellent results from their male breast reduction surgery in Eau Claire, Wisconsin.
Risks of Gynecomastia Surgery
- Chest contour irregularities: There is a risk of chest contour irregularities due to uneven fat removal or skin laxity during the male breast reduction procedure.
- Hormone level changes: Gynecomastia surgery can cause changes in hormone levels, which may lead to further complications such as weight gain or other health issues.
- Surgical excision risks: As with any surgical procedure, there is a risk of infection, bleeding, and scarring associated with gynecomastia surgery.
- Weight gain: Changes in hormone levels caused by gynecomastia surgery may lead to weight gain if not properly monitored and managed post-surgery.
The Expectations of Male Breast Reduction
For gynecomastia patients in Eau Claire, Wisconsin, it is important to maintain a healthy weight before and after the male breast reduction procedure. This will help ensure optimal results and reduce the risk of complications. Patients should also be aware that there may be some swelling and bruising around the chest area following surgery which should subside within a few weeks.
The treatment for gynecomastia typically involves surgical excision of excess tissue and fat from the chest area. This can help create a more masculine appearance and alleviate physical and psychological discomfort associated with gynecomastia. It is important to seek out a board-certified plastic surgeon specializing in gynecomastia to ensure that the procedure is performed safely and effectively.
Recovery and Aftercare of Gynecomastia Surgery
After the gynecomastia surgery is complete, patients typically experience some swelling and bruising around the chest area, which should subside within a few weeks after surgery. Patients should also wear compression garments for several weeks following their procedure in order to reduce swelling and help support their new chest shape as they heal. With proper care and attention, most patients can expect excellent results from their male breast reduction surgery in Eau Claire, Wisconsin.
Patients who have undergone cosmetic surgery for gynecomastia may be able to return to normal activities within a few days of the procedure. However, it is important to follow your doctor’s instructions regarding activity levels during recovery in order to ensure optimal results and minimize the risk of complications. Your doctor may recommend avoiding strenuous activities such as lifting heavy objects or exercising until your body has had time to heal properly.
It is also important to follow any post-operative instructions provided by your doctor in order to ensure a safe and successful outcome. This may include taking medications prescribed by your doctor, avoiding certain foods or beverages, and attending regular follow-up appointments with your surgeon. These steps will help ensure that you are healing properly and that any potential issues are addressed quickly.
Frequently Asked Questions About Gynecomastia Surgery
Why Choose Dr. Ember Ewings
For over a decade, Dr. Ember Ewings has taken pride in delivering excellence in plastic surgical care. She earned her medical degree from the University of Wisconsin-Madison School of Medicine and completed her surgical residency training in plastic surgery at Saint Louis University. Additionally, she gained extensive experience in pediatric and craniofacial surgery during her fellowship at the University of Tennessee – Memphis, and Hôpital Necker-Enfants Malades in Paris, France. Dr. Ewings is also Board Certified by the American Board of Plastic Surgery.
Dr. Ewings has enjoyed caring for patients of all ages from across the upper Midwest, and performs both cosmetic surgical, non-surgical, and reconstructive procedures, and is delighted to be able to provide outreach services in Durand, Wisconsin.
She owns and operates the Plastic Surgery Clinic of Eau Claire in Eau Claire. Prospective patients can reach Dr. Ewings through her online Consult Form, or at her practice, Plastic Surgery Clinic of Eau Claire – 715.833.2116 or 800.456.8222.
Breast Lift
Dr. Ewings customizes each breast lift to match her patient’s unique aesthetic goals for beautifully-shaped, perky breasts and lifted nipples.
Liquid Rhinoplasty
Dr. Ewings can fill in indentations, subtly improve the shape of the nose, and even enhance facial balance by making small adjustments to the nose.
Skin Cancer Treatment
Skin cancer is the most common form of cancer in the United States. More than 600,000 new cases are reported each year.